Donna Thomson has been working with McMaster University to create free online courses for family caregivers. Their latest offering is Infection Prevention and Control for Caregivers and Families.
If you’re worried about keeping someone safe at home or having issues being permitted to visit a loved one in residential care, this is something you should check out. You’ll get a certificate when you complete the course.
You can sign up with for the course through McMaster’s continuing ed program.
This week Caring Across Generations is releasing their 5-part series: Man Enough to Care. The first episode is out now.
If you’d like some guidance on how to approach life’s inevitable changes with curiosity, rather than anxiety, Reimagine has a free program on life’s transitions and transformations.
If you signed up for our group chat program and didn’t get matched, it’s probably because you didn’t include how you’d introduce yourself to someone you’re meeting for the first time.
If you’d like to resubmit (or sneak in to be matched with a group of five or six other people who get it), you can sign up on our Typeform.
Countries around the world have declared caregiving a crisis — some well over a decade ago. The unique medical insurance system and widespread financial precarity of the US make their caregiving crisis unique.
With the hurdles to acquire insurance and the limits to what it covers, is far more likely that the act of providing loving support will come at an unaffordable cost. With a social safety net designed to deter, people must navigate a punitive system in order to access benefits intended to be insufficient.
For all the fighting about what people deserve, everyone agreed: the US medical system was broken.
Then came the novel coronavirus.
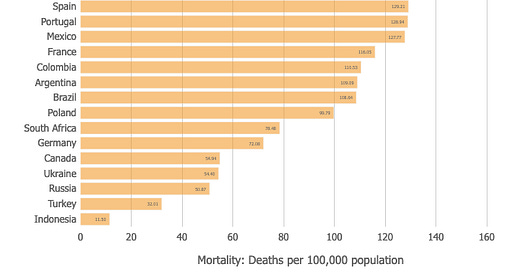
Australia has had 3.64 deaths per 100,000 residents.
The US has had 137.75.

We saw it burn through long-term care facilities and other congregate settings. We became newly aware of who in our lives was high risk. Care work returned to the bad old days where you either surrendered custody to a facility or did it on your own with no help at all.
Caregiving is still a crisis. It’s just a very different crisis today than it was a year ago.
So many of the people who are infected with the novel coronavirus and develop symptoms have seen those symptoms transform, rather than fade away, after their doctors declare them recovered.
There have been 27,683,116 cases of coronavirus in the US. By the time you’re reading this, that number will be higher.
Some of those covid cases are leading to long-haul illnesses.
Professor John Geddes, Director of the NIHR Oxford Health BRC explains, “We know that mental health and neurological problems are quite common after viral infections” which is why he’s leading a UK study on the long-term health complications of COVID-19 survivors.
Post-viral illnesses are not uncommon. It’s estimated that 90% of ebola survivors experienced serious long-term symptoms after recovery.
A study of survivors of the 2003 SARS outbreak found many of them had significant impairment 24 months after “recovery.” It was significant enough that “29.6% of HCW [health care workers] and 7.1% of non‐HCW had not returned to work 2 years after illness onset.”
Another SARS follow-up study found unusually high rates of mental illness and chronic fatigue among survivors.
It’s long been suspected that viral infections can trigger or exacerbate autoimmune disorders. Search “post-x-syndrome” for any viral infection and you’ll unleash an avalanche of blog and message board posts.
Many doctors dismiss post-viral symptoms as hysteria. With the novel coronavirus, doctors are paying attention.
In the UK, they’re seeing around half of coronavirus survivors requiring long-term support. It’s too soon to say how many people will experience long-term symptoms.
In 2019, only 19.3% of disabled people in the US were employed. That was back when only 3.5% of potential workers were unemployed.
What happens as more and more coronavirus survivors are left unable to work and must navigate the US medical system to manage invisible chronic illnesses?
Who takes on the work they performed in their careers, communities, and families?
Who is going to provide care for them?
Who is going to pay the bills?
As so many of us already know, getting disability income in the US involves an epic battle for a measly income:
Long haulers unable to return to work will face more obstacles than they anticipated. Some may find temporary relief under the Family and Medical Leave Act and state-level benefit programs; most will likely turn to their earned Social Security Disability Insurance benefits, which average $1,260.57 per month.
The eligibility determination for disability benefits is notoriously stringent. The initial application typically takes three to five months. Long haulers with proven anatomical damage will often have the objective medical evidence helpful for speedier approval—but those with chronic Covid symptoms that are more difficult to verify through diagnostic tests can expect challenges similar to those of patients with other poorly understood chronic illnesses, like ME/CFS [myalgic encephalomyelitis/chronic fatigue syndrome]. Though it’s estimated that 75 percent of Americans with the condition are unable to work even part-time, as of 2017, the U.S. Social Security Administration reported that only about 13,000 individuals were receiving Social Security disability for a diagnosis of ME/CFS.
…
Long haulers who are approved for disability benefits will automatically qualify for Medicare, regardless of age, but both benefits come with a hitch. The first SSDI check arrives five months after approval, followed by a statutory two-year waiting period for Medicare enrollment.
Coronavirus survivors left disabled and unable to work can look forward to five months without an income and two years without medical insurance, often after a year or more of fighting to get approved for benefits.
People are being pushed out of work because of their health. People are being pushed out of work because of their care work responsibilities.
This is all exacerbating the already drastic economic disparities we see in the US.
This isn’t the post-work world our grandparents predicted:
In 1930, the economist John Maynard Keynes predicted that, by the early 21st century, advances in technology would lead to an “age of leisure and abundance”, in which people might work 15 hours a week.
When my parents were children, the world was predicting that AI would free us from drudgery. Today, we’re warned that AI will lead to vicious competition for increasingly scarce jobs and widespread poverty for those who lose out.
Before the coronavirus, it was already estimated that 1 in 4 Americans had a disability.
Will the increasing proportion of Americans with disabilities and care responsibilities lead to government programs designed to enable, rather than punish? Workplaces that treat humans differently than we treat machines?
So many of us know how adrenaline and dedication can pull us through the demands of care work at first. You can “put life on hold” — sort of — for a little while. And then you burn out.
How many newly minted coronavirus caregivers are about to burn out?